
The Architecture of Care™
Designing Clinical Systems That Support Better Outcomes
Vera Nyonglemuga, FNP-BC, FNP-C, CCRN
Founder, Macvelly Wellness & Medical Services
MBA Candidate, UNC Kenan-Flagler Business School (Forté Fellow)
Healthcare Outcomes Are Not Accidental.
They Are Designed.
Modern healthcare systems are often evaluated through:
quality metrics
throughput targets
efficiency benchmarks
documentation standards
patient satisfaction measures
and operational performance indicators.
Yet many of the most persistent challenges in healthcare delivery continue to involve:
fragmentation
clinician overload
inconsistent continuity
workflow misalignment
cognitive burden
delayed coordination
documentation strain
operational inefficiency
and variability in patient experience.
These issues are frequently approached as:
individual performance problems
staffing limitations
communication failures
or isolated workflow concerns.
However, many of these patterns are structural.
They emerge from the architecture of the systems themselves.
The Architecture of Care™ was developed from the recognition that healthcare outcomes are shaped not only by clinical knowledge or effort — but by how care delivery systems are designed, structured, operationalized, and sustained over time.
What Is The Architecture of Care™?
A Systems-Level Framework for Clinical Care Design
The Architecture of Care™ is a systems-oriented framework focused on understanding how:
operational structures
workflow design
time allocation
communication systems
continuity models
documentation expectations
responsibility distribution
interface design
and organizational incentives
influence:
clinical decision-making
patient experience
continuity
cognitive load
clinician function
and healthcare outcomes over time.
At its core, this framework asks an important question:
What kinds of outcomes are healthcare systems structurally designed to produce?
Because healthcare outcomes are rarely shaped by clinical knowledge alone.
They are influenced by:
the systems clinicians work within
the operational pressures surrounding care
the structure of workflow
the design of time
and the continuity mechanisms supporting decision-making.
Beyond Individual Effort
Many Healthcare Challenges Are Structural
Healthcare systems often depend on extraordinary levels of:
clinician adaptation
cognitive compensation
emotional labor
and invisible coordination work
to maintain continuity and patient safety within increasingly fragmented operational environments.
In many systems, clinicians become the correction layer for:
workflow gaps
communication failures
documentation fragmentation
scheduling inefficiencies
and continuity breakdowns.
Over time, this creates:
cognitive overload
operational strain
inconsistent patient experiences
reduced sustainability
and variability in clinical interpretation and follow-through.
The Architecture of Care™ focuses on identifying and understanding these structural patterns rather than framing them solely as individual shortcomings.
Core Principles of The Architecture of Care™
1. Time Is a Clinical Variable
Time is not simply a scheduling issue.
It directly influences:
diagnostic depth
continuity
interpretation quality
patient understanding
coordination capacity
and longitudinal care planning.
Compressed workflows and fragmented schedules often shape clinical outcomes long before treatment decisions are made.
The Architecture of Care™ recognizes time architecture as a foundational component of healthcare design.
2. Workflow Shapes Clinical Function
Clinical quality does not operate independently from workflow structure.
Workflow influences:
attention allocation
cognitive switching
information processing
coordination reliability
decision fatigue
and continuity preservation.
When workflow systems are poorly aligned, clinicians often spend increasing energy compensating for structural inefficiencies rather than focusing fully on clinical reasoning and patient care.
3. Continuity Requires Structural Support
Continuity is frequently discussed as a value within healthcare systems while operational structures simultaneously undermine it.
Meaningful continuity requires:
protected follow-through
information integrity
responsibility clarity
communication reliability
and sustainable workflow design.
Without structural support, continuity becomes dependent on individual effort rather than system architecture.
4. Cognitive Load Influences Outcomes
Healthcare systems frequently underestimate the impact of:
cognitive fragmentation
task switching
documentation burden
inbox management
information overload
and operational interruption patterns.
Yet cognitive load directly influences:
interpretation quality
decision-making
situational awareness
and long-term clinician sustainability.
The Architecture of Care™ recognizes cognitive burden as an operational design issue rather than solely an individual resilience problem.
5. Healthcare Systems Produce Predictable Patterns
Many recurring healthcare challenges are not random.
They emerge predictably from:
incentive structures
throughput expectations
workflow design
staffing models
documentation systems
communication pathways
and operational priorities.
Understanding these patterns allows organizations to move beyond reactive problem-solving toward more intentional systems design.
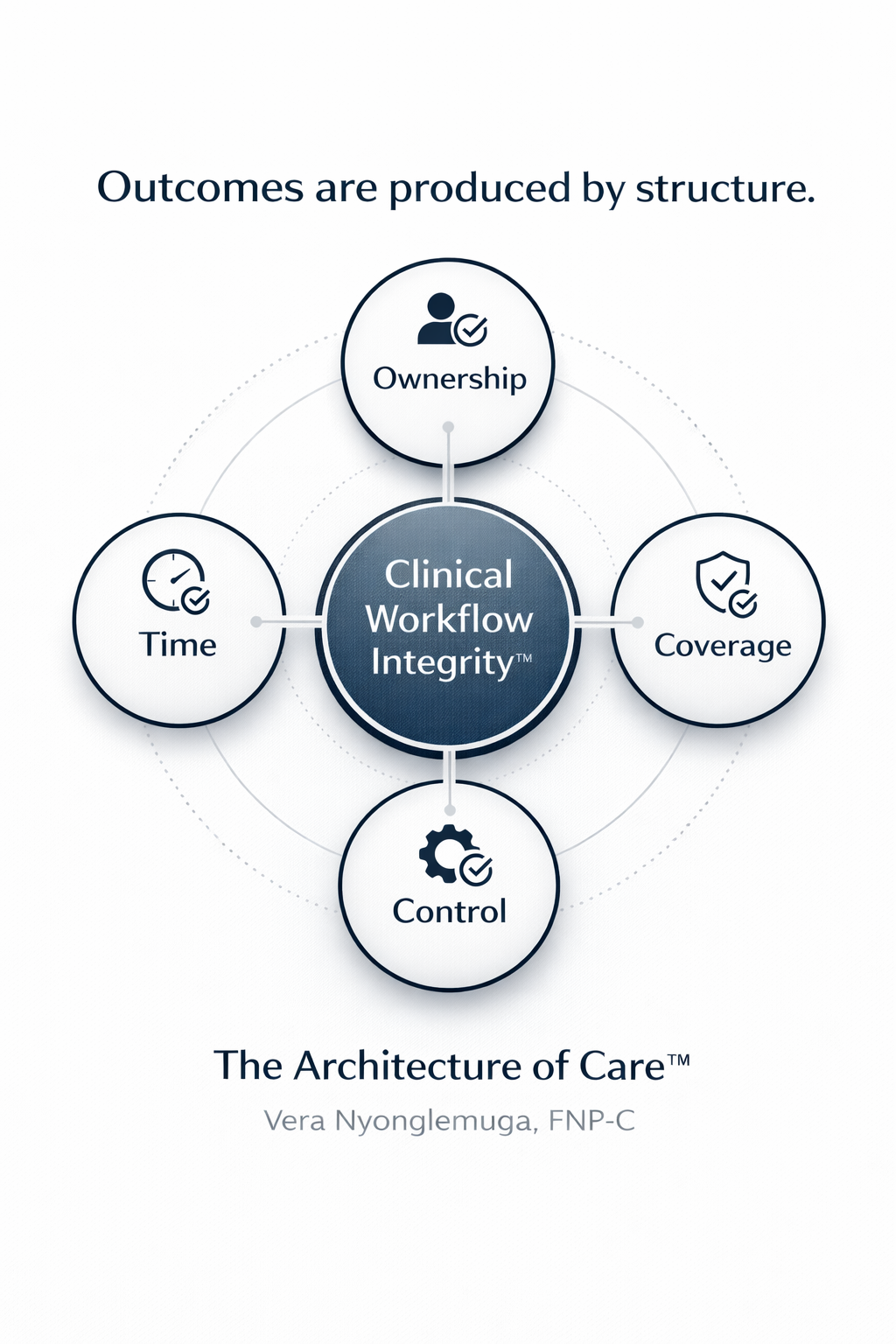
Clinical Workflow Integrity™
A Foundational Concept Within The Architecture of Care™
One of the central concepts within The Architecture of Care™ is Clinical Workflow Integrity™.
Clinical Workflow Integrity™ refers to the degree of alignment between:
clinical intent
workflow structure
and operational interface design.
When these elements remain aligned:
continuity improves
interpretation becomes more reliable
communication stabilizes
cognitive burden decreases
and patient care becomes more sustainable.
When these elements become misaligned:
fragmentation increases
clinician compensation work expands
continuity weakens
variability grows
and systems increasingly rely on individual over-functioning to maintain stability.
Clinical Workflow Integrity™ emphasizes that healthcare quality is influenced not only by clinical expertise — but by the integrity of the systems supporting care delivery itself.
Why This Work Matters
The Future of Healthcare Requires Better System Design
Healthcare systems are entering an era of increasing:
complexity
operational pressure
clinician burnout
workforce instability
technological expansion
AI integration
and growing demands for efficiency and scalability.
Yet sustainable healthcare delivery requires more than increased productivity alone.
It requires:
thoughtful systems design
workflow integrity
continuity preservation
cognitive sustainability
operational alignment
and care models intentionally designed around human physiology and clinical reasoning.
The Architecture of Care™ exists to contribute to these conversations through a systems-oriented lens grounded in both:
frontline clinical experience
and broader organizational thinking surrounding healthcare delivery
Areas of Focus
Current areas of exploration within The Architecture of Care™ include:
workflow integrity
time architecture
continuity systems
clinician cognitive load
operational misalignment
healthcare communication systems
preventive care design
longitudinal care models
patient experience architecture
healthcare sustainability
value-based care operational realities
information fragmentation
AI and clinical workflow integration
and healthcare systems strategy.
Bridging Clinical Care & Systems Thinking
The Architecture of Care™ sits at the intersection of:
clinical medicine
healthcare operations
workflow design
organizational systems
longitudinal care
and human-centered healthcare strategy.
This work is informed by:
frontline clinical experience
systems observation
operational analysis
longitudinal care philosophy
and ongoing study in healthcare strategy and organizational design.
The goal is not simply critique.
The goal is helping create more thoughtful, sustainable, and clinically aligned systems of care.
System Alignment and Outcome Production
These layers function as an interconnected system.
When misaligned:
continuity breaks down
information fragments
decisions become reactive
outcomes vary
When aligned:
care becomes longitudinal
patterns are recognized earlier
decisions are informed
outcomes improve by design
What Changes When Care Is Designed Differently
When systems are structured with alignment and continuity:
Continuity is built into scheduling—not left to chance
Care ownership is clearly defined
Follow-up is structured and expected
Clinical information persists across encounters
Decision-making becomes more precise
Care shifts from:
episodic → longitudinal
reactive → proactive
fragmented → integrated
Application Across Healthcare Systems
The Architecture of Care™ can be applied across healthcare environments to address structural challenges, including:
Designing continuity-centered care models
Aligning workflows with long-term outcomes
Reducing fragmentation across care settings
Integrating metabolic and hormonal health into longitudinal care
Building scalable models for chronic disease and midlife health
Perspective
This framework was developed from within clinical practice—not as an external critique, but from direct experience working inside the systems it seeks to improve.
The challenges observed were not primarily issues of effort, knowledge, or intent.
They were structural.
Improving outcomes requires redesigning the systems that produce them.
Healthcare outcomes are not accidental.
They are designed.
Understanding the structure of care is the first step.
→ Explore how alignment determines outcomes:
Clinical Workflow Integrity™
Looking Forward
Healthcare systems will continue evolving.
The question is whether care models will evolve intentionally — or continue relying primarily on increasing clinician compensation within structurally fragmented systems.
The Architecture of Care™ represents an ongoing effort to better understand:
how healthcare systems shape outcomes
how workflow influences clinical reasoning
how continuity can be structurally preserved
and how care delivery models can become more sustainable for both patients and clinicians over time.
Because healthcare outcomes are not accidental.
They are designed.

