Breast Cancer Under 40 Is Increasing — Let’s Talk About Why
A photograph of a bright, modern clinic waiting room filled with diverse younger women. In the foreground, a Black woman is working on a laptop next to a Hispanic woman holding a clipboard. In the background, a receptionist speaks with another woman near a sign that reads "Mammography Check-In."
For decades, breast cancer was considered a disease that belonged to later life — something most women were taught to worry about after 40, when routine mammograms traditionally begin. But today, the narrative is shifting. More women in their 20s, 30s, and early 40s are receiving a diagnosis long before they ever reach the age of standard screening.
📈 Breast Cancer Is Getting Younger
A large 11-year review found that nearly 1 in 4 breast cancer diagnoses now occur in women ages 18–49 — meaning a significant portion of cases are happening before routine screening even begins.
But what is even more striking:
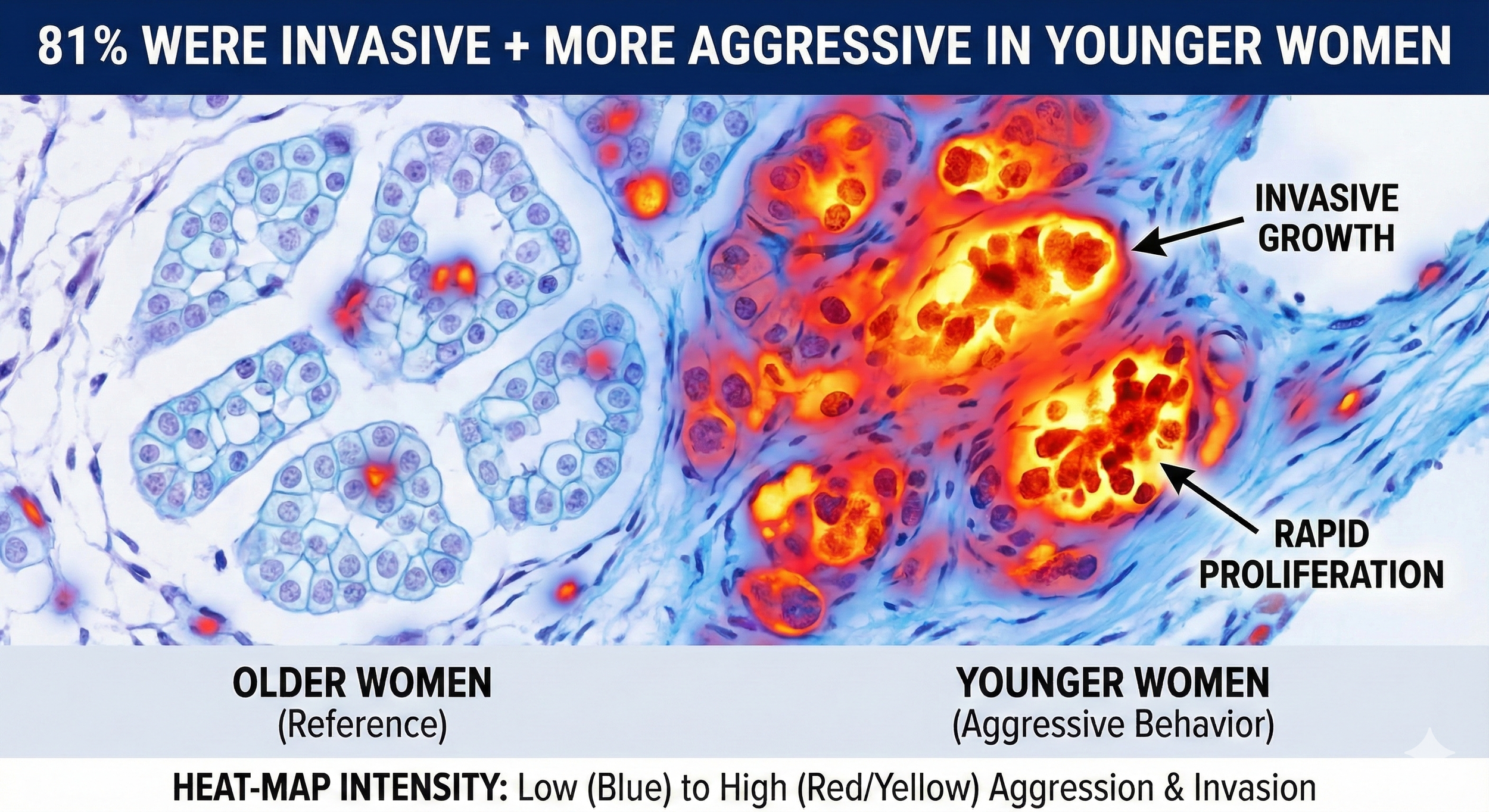
~81% of these cancers were invasive, meaning they had the potential to spread —
and many were classified as biologically aggressive, particularly in women under 40.
A medical illustration using a heat-map style comparison with the header "81% WERE INVASIVE + MORE AGGRESSIVE IN YOUNGER WOMEN." The left side shows calm, blue-stained cells labeled "OLDER WOMEN (Reference)." The right side shows disorganized, intensely glowing red and orange cells labeled "YOUNGER WOMEN (Aggressive Behavior)," indicating rapid proliferation and invasive growth.
Younger women are not just being diagnosed more often — the disease is often more aggressive when it appears.
This should not be a message of fear —
It should be a message of awareness, authority, and early action.
As a clinician, I’m seeing younger women present with symptoms that should never be ignored: persistent breast pain, nipple discharge, changes in breast shape, unexplained lumps, and non-cyclic tenderness. Even more concerning, many women tell themselves, “I’m too young for breast cancer,” and delay evaluation.
If you are in your 30s or early 40s, you might feel dismissed or told you’re too young to worry. But you deserve to know the facts, understand your body, and take proactive steps now.
In this guide, we will break down why younger women are facing this risk, and what every woman needs to know to protect her future.
The truth is: breast cancer is getting younger.
And we need to talk about why.
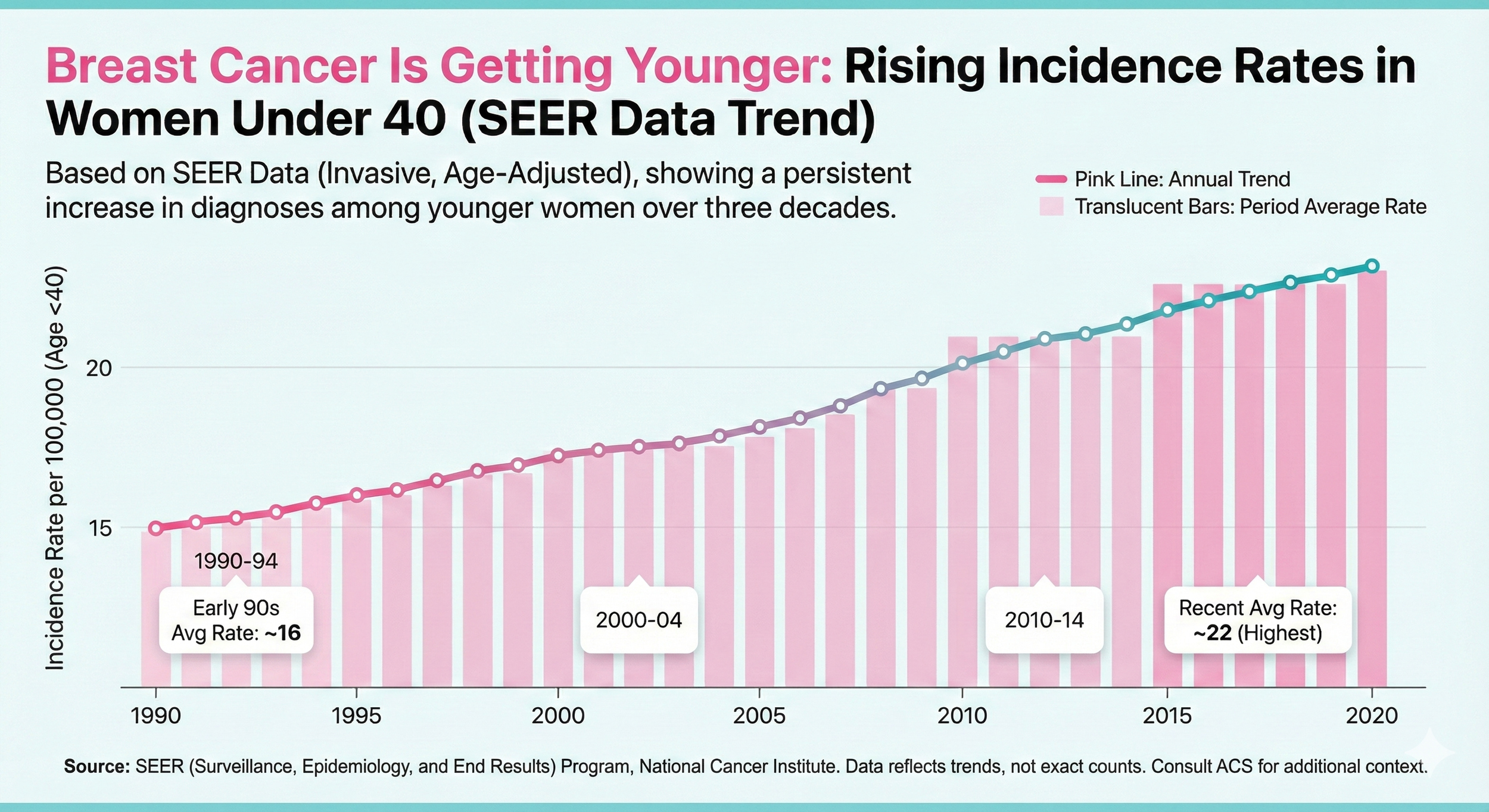
An infographic graph titled "Breast Cancer Is Getting Younger: Rising Incidence Rates in Women Under 40 (SEER Data Trend)." It uses a line graph and bar chart overlaid on a light background to show a clear upward trend in breast cancer incidence among younger women from 1990 (approx. rate of 15) to 2020 (approx. rate of 22).
The Statistics: Why the Urgency Is Real
Breast cancer has always been a risk, but the patterns are changing.
Earlier Onset: We are seeing more cases diagnosed in women in their 30s and 40s than in previous generations.
Aggressive Nature: Breast cancer diagnosed at a younger age is often biologically more aggressive and harder to treat.
The Unseen Disparity: This trend hits women of color harder. Black women are often diagnosed later, partly due to systemic screening delays and misdiagnosis, making early awareness absolutely vital.
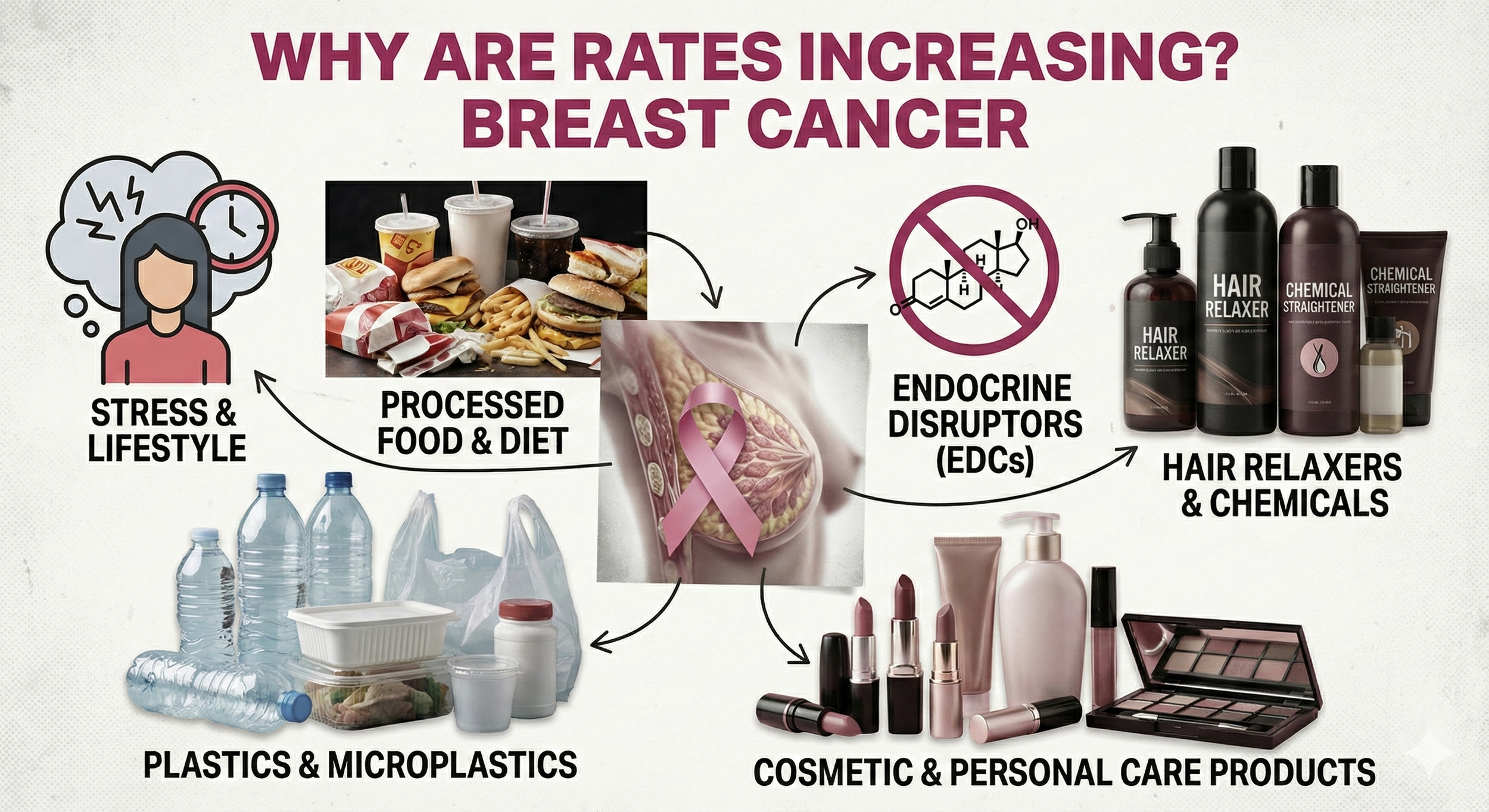
A collage infographic titled "WHY ARE RATES INCREASING? BREAST CANCER." It connects various environmental and lifestyle factors to breast cancer risk using arrows pointing to a central image of a breast with a ribbon. The factors included are Stress & Lifestyle, Processed Food & Diet, Endocrine Disruptors, Plastics & Microplastics, Hair Relaxers & Chemicals, and Cosmetic & Personal Care Products.
Why Are Younger Women Being Diagnosed More Often?
Research from multiple cancer registries shows a steady, concerning rise in breast cancer cases among women under 40. While the exact cause isn’t singular, science points to several contributing factors — many of which intersect with modern lifestyle, environment, and hormonal patterns.
1. Hormonal Disruptions & Earlier Puberty
Why girls are entering womanhood sooner — and what this means for breast cancer.
Breast cancer risk is deeply influenced by lifetime estrogen exposure.
The earlier breast tissue is stimulated by estrogen, the longer it remains hormonally active across a woman’s life. This makes early puberty one of the most important — and least discussed — contributors to rising breast cancer rates in young women.
Over the last three decades, global data shows:
📌 Average age of first menstruation has dropped from 12.5 to 11 years in many regions
📌 A Pediatrics (2020) review notes African American girls enter puberty nearly 1 year earlier than white peers
📌 Early breast development before age 10 increases lifetime breast cancer risk by 20–30%, independent of genetics
This trend is not merely biological drift — it is environmental influence.
What’s driving earlier puberty?
Researchers cite a multifactorial cause:
Endocrine-disrupting chemicals (EDCs) that mimic estrogen
Higher childhood body fat percentages (adipose produces estrogen)
Ultra-processed food consumption altering insulin + leptin signalling
Chronic stress + adverse childhood experiences (ACEs) accelerating maturation pathways
Reduced outdoor physical activity + increased sedentary play
The result is early estrogen exposure + longer lifetime hormonal cycling, which leaves breast tissue proliferating, dividing, responding — for more years than previous generations.
Why this matters for breast cancer:
Early puberty → longer estrogen window → more cell replication → more opportunities for DNA mutation and carcinogenesis.
And because modern girls enter puberty earlier but are not having children earlier (due to cultural and socioeconomic shift), their breast tissue remains unprotected by full-term pregnancy for years longer — a biological gap we’ll explore in the next section.
2. Environmental Toxins & Endocrine Disruptors
One of the most unsettling findings across recent cancer research is how deeply our modern environment interacts with female biology — particularly estrogen-sensitive tissues like the breast. Breast tissue is hormonally driven, responsive, and vulnerable. When synthetic chemicals act like estrogen or interfere with hormone signaling, the breast is often where the damage quietly settles.
These are known as endocrine-disrupting chemicals (EDCs) — compounds found in everyday life that can mimic estrogen, block hormone receptors, or alter hormonal metabolism.
Common Chemical Sources + How They Influence Hormones
Many of the endocrine-disrupting chemicals linked to breast cancer in younger women are not exotic or rare — they are woven into everyday life. They sit in our kitchens, our personal care routines, the products we buy, the dust in our homes. And most women have been exposed to them since childhood.
One of the most well-known is BPA (and its replacements like BPS/BPF), commonly found in food packaging, receipts, plastic containers, and the linings of canned foods. BPA can mimic estrogen inside the body, binding to hormone receptors and stimulating breast cell growth — a concerning mechanism when exposure begins early in life.
Phthalates are another significant category. These chemicals are widely used to make fragrances last longer and plastics more flexible, meaning they are often found in perfumes, body sprays, lotions, cosmetics, vinyl items, and many conventional hair and personal care products marketed heavily to women of color. Phthalates disrupt reproductive hormones and can accumulate in fat tissue over time, slowly layering exposure year after year.
Then there are PFAS — often called “forever chemicals.” These appear in nonstick cookware, fast-food wrappers, water-resistant jackets, stain-proof furniture, and even drinking water in certain regions. They are incredibly persistent, remaining in the body for decades, and increasing research links them to tumor-promoting activity.
Pesticides and herbicides found in non-organic produce and lawn treatments are also capable of influencing breast tissue. Some have been shown to behave like estrogen within the body, and multiple studies associate pesticide exposure with estrogen-receptor-positive breast cancer.
Finally, flame retardants — used in furniture, mattresses, children’s sleepwear, and everyday household dust — can alter thyroid function and disrupt hormone-related gene expression. Because breast tissue is highly responsive to shifts in the endocrine system, this type of interference may change cellular behavior over time.
Why This Matters
These exposures don’t cause cancer overnight — they accumulate quietly, sometimes from infancy onward. By adolescence, before a girl has any concept of risk, she may already have a measurable hormonal burden. And because breast density is naturally higher in younger women, breast cells may be more reactive to endocrine disruption during these years.
What research suggests:
📌 A 2023 JAMA Oncology review reported that women with higher urinary BPA and phthalate levels had more frequent hormone-positive tumor patterns.
📌 A 2024 NIH environmental study revealed that Black women had disproportionately higher levels of phthalates and parabens — often due to product targeting in beauty/hair industry marketing.
(This is a cultural factor the media rarely talks about.)
📌 PFAS chemicals have now been detected in 97% of Americans, with growing evidence linking them to breast and ovarian malignancy pathways.
This is not fear — this is information. Awareness becomes power only when paired with action.
Once women understand where exposures come from, they gain the power to change them.
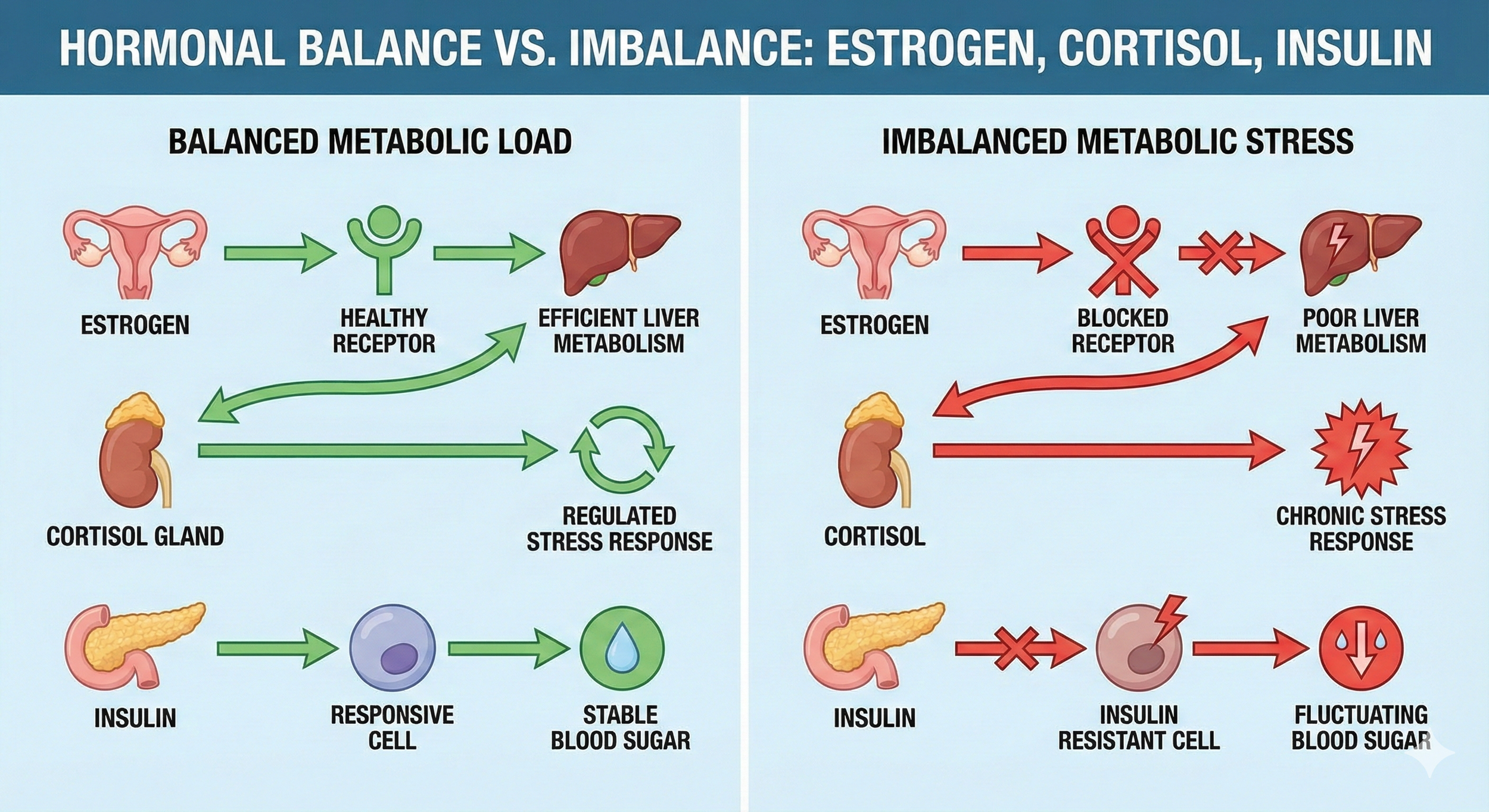
3. Chronic Stress & Metabolic Load — The Hidden Driver We Aren’t Talking About Enough
A two-panel medical diagram comparing "HORMONAL BALANCE VS. IMBALANCE." The left panel, "BALANCED METABOLIC LOAD," shows healthy green pathways for Estrogen, Cortisol, and Insulin leading to efficient metabolism and regulated responses. The right panel, "IMBALANCED METABOLIC STRESS," shows red, broken pathways leading to blocked receptors, poor metabolism, chronic stress, and insulin resistance.
When we talk about breast cancer in young women, we often look outward — at chemicals, genetics, hormones, environment. But there is another factor woven into the lives of modern women so deeply it becomes invisible:
Chronic stress.
Not momentary overwhelm — but ongoing, unrelenting stress physiology.
Younger women today are carrying workloads that previous generations rarely faced simultaneously: demanding careers, childcare, aging parents, economic stress, academic pressure, relationship labor, identity pressure, constant digital stimulus — all while being expected to function flawlessly.
The result is a body stuck in sympathetic overdrive.
Instead of cycles of stress + recovery, many women are living in:
elevated cortisol for months or years
disrupted sleep patterns
insulin dysregulation
increased inflammatory cytokines
reduced immune surveillance against abnormal cells
This combination is now being referred to by researchers as metabolic load — the cumulative biological stress a body holds over time.
What does this mean for breast cancer?
Cortisol is not just a “stress hormone.” It is a system regulator, influencing immune function, estrogen metabolism, insulin signaling, and inflammation pathways — all of which are central to tumor development and progression.
Scientific insights aligned with this include:
📌 Chronic cortisol elevation increases aromatase activity, raising estrogen levels in breast tissue — especially relevant for estrogen-receptor-positive (ER+) tumors.
(Endocrine Reviews, 2022)
📌 Women with high perceived stress scores showed accelerated telomere shortening, an aging marker linked to increased cancer susceptibility.
(PNAS, 2019)
📌 Dysregulated stress hormones impair natural killer (NK) cell function, reducing the body’s ability to identify and destroy mutated cells early.
(Nature Immunology, 2021)
📌 Stress disrupts circadian rhythm — particularly in shift workers — which the WHO now classifies as a probable carcinogen related to breast cancer.
(International Agency for Research on Cancer, 2023)
This means stress is not “emotional.” Stress is cellular.
And when metabolic load remains high for years, the body becomes inflamed, insulin-resistant, and hormonally dysregulated — a metabolic landscape where cancer can more easily take root.
Stress + Metabolism = A Mechanism, Not a Mystery
Chronic stress influences cancer risk through four main biological pathways:
Hormonal Overdrive
Cortisol dysregulation increases estrogen dominance, elevates prolactin, and alters progesterone balance — shifting breast tissue into a more proliferative state.
Impaired Immune Detection
Stress reduces the activity of T-cells + NK cells responsible for early tumor surveillance.
Systemic Inflammation
High metabolic load leads to ongoing low-grade inflammation, a recognized hallmark of cancer development.
Insulin Resistance & Weight Gain
Cortisol increases glucose retention, abdominal fat storage, and insulin spikes — and insulin itself can act as a growth signal for tumor cells.
This is why two women can have similar lifestyles, diets, or genetics — and yet one develops disease and the other does not.
It’s not always what we see.
Sometimes it’s what we carry.
Why Younger Women Are Particularly Vulnerable
Women under 40 are living in the intersection of:
historically high stress exposure
less sleep than recommended (avg 5.5–6.2 hrs)
higher stimulant intake (caffeine, energy drinks)
less restorative rest, community support, and slow living
increased perfectionism + achievement pressure
higher fertility-related hormonal load
Add to that cultural expectations for women — especially Black women and women of color — to remain strong, resilient, uncomplaining, endlessly productive.
Stress becomes normalized.
Pain becomes minimized.
Symptoms become dismissed.
And biology responds accordingly.
4. Delayed Childbearing & Fewer Lifetime Pregnancies
Modern milestones have shifted — so has breast biology.
Biologically speaking — and separate from personal choice or fertility autonomy — pregnancy and breastfeeding profoundly shape breast tissue in ways that affect cancer risk.
Historically, women gave birth younger and more often.
Today, the pattern looks very different:
Average age of first childbirth has risen from 24 (1990s) → 30+ today
Many women have only one child or none by choice or circumstance
Breastfeeding duration is shorter than biologically expected
Why this matters physiologically:
During the first full-term pregnancy, breast cells undergo terminal differentiation — meaning they become more mature, more stable, less likely to mutate. This process completes around week 34 of pregnancy:
📌 Full-term pregnancy decreases long-term breast cancer risk by ~30%
📌 Each breastfeeding year reduces risk an additional 4–7%
(The Lancet Meta-analysis, 2012; reaffirmed in 2023 review)
Without pregnancy — or with pregnancy later in life — breast cells remain more immature and estrogen-responsive for longer, and thus more vulnerable to carcinogenic triggers.
Delayed childbearing is not a “problem” — it’s a biological reality of modern living.
Women are pursuing education, careers, financial stability, self-growth — choices that should never be pathologized. But understanding this shift helps us better design screening strategies and prevention frameworks.
Because knowledge is not about guilt — it is about agency.
5. Lifestyle Patterns: Movement, Diet, Alcohol
A candid photograph showing a woman in a cafe looking overwhelmed and stressed. She is holding her head in her hand, staring at complex spreadsheets on a laptop. It is a rainy day outside the window, and she appears exhausted, representing urban work stress and burnout.
The daily decisions that quietly tilt risk up or down.
Breast cancer does not emerge from a single cause. It reflects the sum of biological, environmental, and lifestyle influences over years. Among modifiable factors, three stand out most consistently across global research:
A) Movement & Metabolic Health
Physical activity is one of the strongest modifiable breast cancer protective factors.
Regular movement lowers circulating estrogen + insulin
Exercise reduces inflammatory cytokines + improves immune surveillance
Even walking 30 minutes daily reduces risk by ~13–18%
(Harvard School of Public Health, 2021)
Resistance training is particularly powerful, increasing muscle mass → improving insulin sensitivity → decreasing aromatase activity in adipose tissue → lower estrogen dominance.
Sedentary lifestyles — which now affect most women under 40 who work desk-based jobs — do the opposite.
B) Diet Patterns — Not Rules, But Biology
No single diet prevents cancer — it is pattern, not perfection that matters.
Evidence supports:
High-fiber & cruciferous vegetables improve estrogen metabolism
Omega-3 rich foods reduce inflammation & upregulate BRCA-protective genes
Lower intake of ultra-processed foods reduces insulin + oxidative stress
Plant-forward eating correlates with lower overall breast cancer incidence
(International Journal of Cancer, 2023)
Highly processed diets spike insulin → insulin acts as a growth signal.
High saturated fat + low micronutrient intake → oxidative DNA damage.
The modern woman’s diet is overfed but under-nourished — and cancer flourishes in that dysfunction.
C) Alcohol — The Most Consistent Risk Factor Women Underestimate
Even moderate alcohol intake increases breast cancer risk dose-dependently.
3–6 drinks per week → 15% increased risk
One drink per day → 30% increased risk
More than one drink/day → risk rises sharply
(American Cancer Society, 2024 update)
Why? Alcohol increases:
Aromatase activity → more estrogen circulation
Oxidative stress → DNA mutations
Acetaldehyde toxicity → carcinogenic load
For women genetically predisposed or experiencing high stress, alcohol's biological impact is even more magnified.
Prevention & Metabolic Regulation Protocol
Evidence-Based Strategies to Reduce Risk and Strengthen Breast Health in the Modern World
Prevention is not about control — it is about capacity.
Capacity to metabolize hormones safely.
Capacity to resist carcinogenic stress.
Capacity to maintain immune surveillance.
Capacity to repair cellular injury rather than accumulate it.
We cannot change genetics or the era we live in, but we can change the biological landscape inside us — the soil in which cancer either struggles or thrives.
Below is a science-grounded, practical prevention framework women can implement across metabolism, hormones, sleep, diet, stress, and environment.
A) Supporting Hormone Balance + Estrogen Detoxification
Estrogen is not the enemy. Stagnant estrogen is.
The goal is not less estrogen — it is better metabolized estrogen.
Breast tissue is protected when estrogen is processed through the 2-OH pathway, rather than the 4-OH or 16-OH pathways linked to tumor proliferation.
How to support this:
Nutrition-based detoxification
(Phase I & II liver metabolism)
Cruciferous vegetables 4–6x/week
(broccoli, kale, cabbage, Brussels sprouts — rich in sulforaphane + DIM)Consume 25–35g fiber/day for estrogen elimination
Add 1–2 tbsp ground flaxseed daily (phytoestrogens that compete with stronger estrogen)
Prioritize hydration to support bile clearance
Journal of Nutrition, 2022 — women consuming crucifers showed a shift toward protective estrogen metabolites.
Supplements With Evidence
(For education — not blanket prescriptions)
DIM (Diindolylmethane) → improves estrogen metabolite ratio
Calcium-D-Glucarate → supports Phase II conjugation
Sulforaphane extract → upregulates detox enzymes (Nrf2 pathway)
Clinical note: Supplements should be personalized and physician-guided, especially for women with hormonal disorders or liver disease.
B) Metabolic Stability — Lowering Insulin, Inflammation, and Aromatase Activity
Breast cancer development is strongly linked to metabolic dysregulation — particularly insulin resistance, chronic inflammation, and excess adipose aromatase activity.
Core Strategies:
Movement
150 minutes/week moderate exercise
2–3 days resistance training
Break up sitting every 45 minutes
Even light walking post-meals improves glucose disposal by up to 30%.
📎 JAMA Internal Medicine (2021) — women with high physical activity had 18–25% lower breast cancer incidence.
Metabolic-Nourishing Nutrition
Protein 25–30g per meal → stabilizes insulin + reduces hunger
½ plate vegetables (especially crucifers + leafy greens)
Healthy fats (olive oil, avocado, fatty fish) → reduce inflammation
Minimize ultra-processed foods & reduce added sugar
Aim for slow glucose curves, not perfect meals
Alcohol Minimization Framework
Instead of all-or-nothing, use a conscious moderation scale:
0–2 drinks/week = lowest measurable risk
3–6 drinks/week = noticeable increase
>6 drinks/week = high-risk metabolic territory
C) Nervous System Regulation — The New Cancer Prevention Pillar
Stress is not emotional — it is biochemical.
Unregulated stress → chronic cortisol elevation → increased insulin + estrogen → increased breast cancer vulnerability.
Evidence-rooted interventions:
Daily Parasympathetic Activation
Diaphragmatic breathing (5 minutes)
Mindfulness-based stress reduction
Yoga, tai chi, or gentle somatic movement
Grounding practices (sunlight, nature exposure)
Harvard Mind-Body Institute (2020) — daily relaxation response practice reduced inflammatory markers by 15–22%.
Sleep as a Biological Repair System
Sleep controls melatonin — and melatonin inhibits tumor growth.
To strengthen circadian rhythm:
Goal: 7–8.5 hours nightly
Dim lights 2 hours before bed
No screens 60–90 minutes before sleep
Magnesium glycinate, tart cherry, and early sunlight exposure may help regulate rhythm
Shift work, night shifts, or chronic bedtime irregularity significantly increases breast cancer odds — particularly for women under 40.
D) Environmental Exposure Reduction
Not perfection — exposure subtraction over time.
Simple foundational swaps:
Glass or stainless for food storage
Filtered water (especially PFAS-reducing filters)
Clean cosmetic + personal care products
Avoid heating food in plastic containers
Declutter fragrance and aerosol products
Environmental Health Review, 2023 — women with lower EDC load had more favorable estrogen metabolite patterns.
E) Screening, Self-Advocacy, and Early Detection
Young women are often dismissed — so advocacy matters.
Breast monitoring plan:
Monthly self-breast awareness (not rigid exams — awareness of change)
Annual clinical exam
Ask for imaging if anything feels wrong (even under 40)
Family history → consider genetic risk consultation
BRCA-positive or strong family history → earlier screening may save life
If a provider dismisses symptoms — women must feel empowered to request second opinions.
Early detection is not luck — it is literacy.
F) Cultural Integration for Women of Color
Black women face:
Higher phthalate exposure
Higher stress load and care labor
More aggressive tumor patterns
Later diagnosis and less timely treatment
Prevention strategies should center:
Rest as resistance
Clean beauty swaps aligned with textured-hair needs
Advocate early — don’t wait for severity
Build community support instead of operating in silent strength
Strong Black Woman Syndrome may be heroic — but it is not always protective at the cellular level.
Rest is medicine.
Boundaries are prevention.
Silence is not strength.
Advocacy is survival.
Who Is Most at Risk Under 40?
Not for fear — for awareness, readiness, and early action.
Breast cancer in young women is still statistically less common than after 50 — but when it happens, it is often more aggressive, faster-growing, and diagnosed later, simply because women under 40 are not routinely screened.
Certain groups carry higher risk and warrant earlier vigilance and self-advocacy:
Genetic + Familial Risk
Women with:
BRCA1 or BRCA2 gene variants
First-degree relative with breast or ovarian cancer
Family history diagnosed under age 50
Multiple relatives with breast/prostate/pancreatic cancer
📌 BRCA1 mutation → up to 72% lifetime breast cancer risk
📌 BRCA2 mutation → 69% lifetime risk
(Nature Genetics, 2021)
Hormonal + Reproductive History
Higher risk in women who:
Began menstruation early (<11 yrs)
Have never been pregnant or gave birth after 30
Did not breastfeed
Have prolonged hormonal contraceptive exposure (some forms)
Not condemnation — information.
Lifestyle + Metabolic Factors
Increased susceptibility with:
Obesity or weight gain in adulthood
Chronically elevated stress + poor sleep
Low physical activity
Regular alcohol intake
Metabolic health has emerged as equally important as genetics.
Environmental Exposure
Higher risk in women with:
Frequent use of fragrance-heavy hair/beauty products
High exposure to plastics, PFAS, pesticides
Occupational exposure (lab, medical, factory, salon workers)
Race & Inequity — A Necessary Truth
Black women under 40:
Develop breast cancer more frequently
Are diagnosed later
Are more likely to have triple-negative and aggressive tumors
Face greater medical dismissal and undertreatment
Not because Black biology is flawed —
but because the system is.
Awareness is armor.
Preparation is power.
Symptoms Young Women Should Never Ignore
A bold, high-contrast checklist infographic titled "SIGNS OF BREAST CANCER WOMEN SHOULD NEVER IGNORE." It uses red and amber icons to list key symptoms: New lump or thickening, nipple discharge, skin changes (dimpling), nipple retraction, redness/scaling/rash, change in size or shape, and persistent breast pain.
Because "You're too young" has delayed far too many diagnoses.
Most young women are told their symptoms are hormonal, benign, or imagined.
Too many wait months — or years — before being imaged.
These are signs that require evaluation promptly:
Breast or nipple symptoms
A lump, thickened area, or new density
Skin dimpling (orange peel appearance)
Nipple inversion or change in shape
Spontaneous or bloody discharge
New asymmetry between breasts
Pain that persists or worsens
Not all pain is cancer — but consistent, localized pain deserves attention.
Changes in skin or texture
Redness, rash, darkening, scaling
Warmth or swelling without infection
Skin tethering or pulling
Breast swelling after injury
If swelling persists beyond healing → investigate.
Underarm or collarbone lumps
Swollen lymph nodes can be an early sign.
Unexplained systemic symptoms
Unintentional weight loss
Persistent fatigue
Bone pain or shortness of breath (late signs)
📌 If a provider dismisses symptoms because of age — ask for imaging anyway.
📌 Ultrasound is often more effective than mammogram in dense young tissue.
📌 Young women have a right to second opinions.
Your body is speaking — you never need permission to listen.
What You Can Do Right Now
Three steps to lower risk, strengthen immunity, and increase early detection — starting today.
We end not with fear, but with empowerment in motion.
You do not need to overhaul your life.
You need only begin.
Step 1 — One Daily Habit for Hormone Metabolism
Choose only one:
1–2 tbsp ground flaxseed daily
A cruciferous vegetable every day
Replace plastic food storage with glass
Drink water before coffee each morning
Small + consistent > dramatic + unsustainable.
Step 2 — Protect Your Future Self
Learn your family history
Document your personal risk profile
Start monthly breast self-awareness
Calendar reminder → non-negotiable.
Step 3 — Reduce One Source of Metabolic Stress
Choose what feels possible:
10-minute daily walk after meals
Alcohol-free weekdays
Phone off 60 minutes before bed
Replace fragrance products with clean alternatives
5 minutes breathing before sleep
Every biological improvement — glucose, cortisol, inflammation, estrogen clearance — stacks like compound interest.
You are not powerless.
You are participating.
We Are Not Too Young. We Are Not Too Late. We Are Not Helpless.
A professional wellness consultation scene featuring a woman in a mint green blazer speaking confidently with a client across from her. The setting is calm, bright, and modern with natural lighting, plants, a laptop, and notes visible — creating an atmosphere of trust, education, and patient-centered care. The image represents supportive breast health guidance, preventive care, and women empowering women through informed conversation.
Breast cancer under 40 is not an anomaly anymore —
it’s a warning signal from the body of a generation.
A generation exposed to more chemicals, more chronic stress, more metabolic strain, later pregnancies, earlier puberty, fewer buffers, more expectation, and less rest.
This is not coincidence.
This is biology in real time.
But biology is not destiny.
Because when women understand the mechanisms behind their risk — when we see the systems, the products, the pressures, the delay in diagnosis — we stop whispering. We stop waiting. We stop being told we are “too young” to advocate for ourselves.
We stand differently.
We choose differently.
We demand differently.
This article is not just information — it’s a call to action.
No woman should be told to wait and see.
No woman should dismiss her breast pain.
No woman should feel too young to be taken seriously.
Not anymore.
We deserve providers who listen, research that includes us, screening that reflects our lived reality — not outdated norms. We deserve environments that don’t load our cells with endocrine disruptors, beauty industries that don’t target us with cancer-linked ingredients, workplaces that don’t glorify exhaustion over longevity.
We deserve medicine that evolves with the truth —
and young women deserve to be seen.
Breast cancer in our 20s and 30s is not rare enough to ignore.
And we are not silent enough to let it continue.
Knowledge is power — but action is prevention.
So go forward aware.
Go forward educated.
Go forward unafraid to demand imaging, testing, clarity.
Because early detection is not luck — it is literacy.
And survival is not chance — it is preparation.
This is not fear-based health.
This is informed reclamation.
We are the generation that stops saying, “This doesn’t happen to women like me.”
We are the generation that makes sure fewer women ever have to say, “I wish I had known sooner.”
📥 Breast Health Prevention & Action Guide — Free Download
Take this knowledge with you.
Share it. Save it. Start applying it.
This downloadable guide includes:
✔ Risk assessment checklist
✔ Symptoms no woman under 40 should ignore
✔ Daily prevention habits that reduce risk over time
✔ Hormone, metabolism & lifestyle support strategies
✔ Environmental exposure reduction
✔ Stress + sleep support for breast protection
⬇ Click to Download the Breast Health Prevention & Action Guide
This conversation cannot end in your mind — it has to continue in your life.
If this article gave you clarity, urgency, or even discomfort, let it move you into action. Share this with another woman under 40. Start a prevention habit today. Book a Free Clarity Consultation if you want support tailoring a plan to your hormones, metabolism, or breast health risk.
Knowledge saves lives —
but only when we do something with it.
You are not too young.
You are not too late.
You are not powerless.